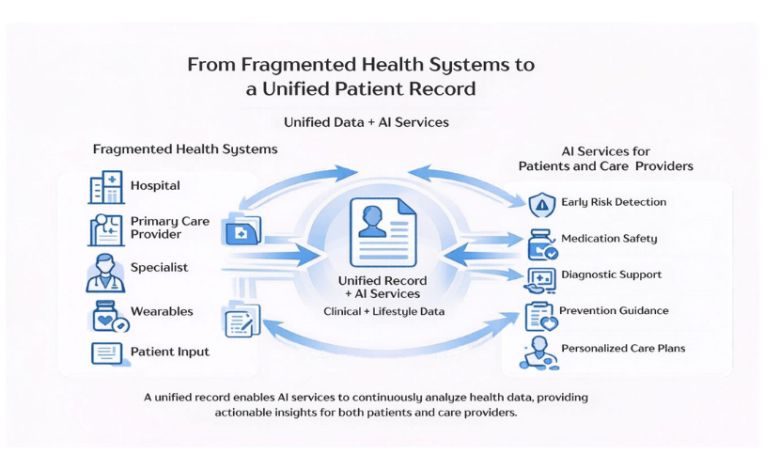
The United States healthcare industry consumes approximately 18% of U.S. gross domestic product, reflecting a model that’s overwhelmingly structured around healthcare’s systems rather than around the patients they serve.
Thousands of databases store fragmented and erroneous data, presenting an opportunity to create a single, cleansed version of the truth for every patient that also includes their family history.
While the industry has gravitated to using AI for diagnostics and identifying drug incompatibilities, the most important component is good data. The old adage, “garbage in, garbage out” is particularly true in the medical space, since data is stored in many systems of records with no single version of the truth. This translates into inaccurate AI system data. Without the complete and accurate medical records and other associated wellness data, the AI system’s capabilities will only be as good as the data it is being fed. This is also true of the care provider, since their diagnosis is only as good as the data they are basing it on.
This poor data quality contributes to medical errors, delayed or inaccurate diagnoses and inconsistent clinical outcomes, ultimately driving up healthcare costs.
Significant improvements in diagnostics capabilities, preventative care, drug research and clinical trials can only be made available if the market first solves this problem of fragmentation and creates a single and complete version of the truth.
Current use of AI in healthcare – Let’s dig a little deeper
There are numerous claims of AI benefits in medicine: improved diagnostics and early detection; administrative workflow efficiency; accelerated research and drug discovery; and enhanced experiences for patients and providers are just a few.
The use of consumer AI search has empowered patients to understand their own symptoms and secure valuable feedback on potential solutions to their health concerns in a much more clear and interactive manner than traditional web search. With this knowledge, patients are better positioned to take steps toward improved health.
The drawbacks
While AI has long been touted as the savior of modern medicine by solving complex diagnoses and delivering early critical warning systems that tackle morbidity concerns, it mostly helps providers with patient charting to meet insurer coding demands.
While this may seem convenient, it has long been criticized by patients and doctors alike for turning doctors into scribes and minimizing their time with patients. Additionally, these benefits often fall short or are realized only within a single health system, and they’re not inclusive of all caregiver data for a given patient. Further, they center on the health system rather than focusing on the patient, their full life-care data and preventative needs.
However, the real issue encompasses the daily challenges to patients and doctors in keeping the vast amount of patient information in an accurate, meaningful, accessible and impactful way.
What’s needed? A single source of complete and accurate patient truth.
Barriers to using AI in healthcare
While utilizing AI is critical, barriers exist that prevent this transformation.
Our data is fragmented
Patients and providers attempt to use data from multiple systems, including hospitals, clinics, portals and labs. This data is provided from the patient directly, with limited automated feeds, and therefore is usually limited in scope and fraught with errors. Because this information is siloed in many systems of record and in the head of the patient, it’s difficult to arrive at a single source of truth.
Solutions are not patient-centric
Not only can patients not see their records in language they understand, but they are also unable to update or correct their personal information or share symptoms and context before they visit a healthcare provider. Thus, both patients and their care providers spend a significant amount of time filling out forms and answering questions versus focusing on quality time between the doctor and his patient.
We focus on treatment
There are a myriad of aspects that contribute to our health profile. Our medical record holds information about our medical conditions, medications and lab results and are focused on treatment but do not focus on preventative measures. Our diet and workout habits are contributing factors to our health, yet they’re rarely discussed, let alone included in a health profile.
We lack a continuous feedback loop
Many foods and their ingredients drive chronic issues; drugs and combinations of drugs can cause problems; and many behaviors and associated patterns are related to poor outcomes. Yet these factors are not looked at holistically or offer insights into patient health. Nor is their cause and effect performed on the aggregate data to determine how to change the food supply or drug protocols to become more preventive and reduce the number of chronic illnesses.
A single source of truth: Solving one of healthcare’s biggest problems
First and foremost, implementing a single healthcare network across the entire medical industry will provide a complete single version of the truth. This, in conjunction with an AI system that leverages data, will save time, money and lives.
A patient-centric healthcare network enables a complete, clean and accurate individual health record, and it’s how AI can drive clear treatment and prevention-focused outcomes. Ultimately, this shifts our health focus from treatment to prevention, thus reducing chronic illnesses and substantially reducing costs and saving lives.
It brings the information to the patient so they can make better decisions that fit into their lifestyle and healthcare goals. The convenience and strength of personalized “all about you” advice makes it easier to manage one’s health to achieve the desired outcomes.
Without a single source of truth, patients will continue piecing together their health records across providers, resulting in forgotten and missing information, especially in the time of most need: acute, urgent and emergent care.
Additionally, families miss out on the immense benefits of having a complete, accurate and clean family medical history. Imagine being able to inherit a full medical family history that AI can use to provide effective prevention-level guidance throughout life.
A single patient record allows authorized healthcare providers and their patients to instantly access patient data to create accurate and complete medical histories, make better patient care decisions, prescribe fewer redundant tests and procedures and lower the chance of medication mix-ups and diagnostic errors.
By bringing together clinical, pharmaceutical, laboratory, wellness and administrative data into one system, a reliable foundation for coordinated care, operational efficiency and system-wide cost reduction is established and better engages patients in their own preventative care.
How AI will support revolutionary change in the industry
To improve health outcomes and reduce rising costs, the focus should shift from treating illnesses to emphasizing prevention. This change needs medical records to do more than just show when someone is sick. They need to include family history and an AI system to suggest the right medical care, dietary and exercise programs needed to support prevention. This solution should not only suggest the right prevention measures but it should track and adjust programs based on changes in personal goals, medical protocols and associated diet and exercise plans.
The AI system needs to support learning models focusing on the main reasons behind conditions like obesity, heart disease, diabetes and some cancers by requesting changes in the food supply, new drug research and encouraging activity. These learning models moving the population into a preventative care model is the best way to reduce long-term healthcare costs and enhance community health.
AI serves as an augmentation layer within the healthcare ecosystem to enhance clinical judgment, not to replace it, and increase patient engagement in their treatment-based and preventative care. By continuously analyzing complete and accurate patient data, population-level outcomes and real-world evidence, AI systems can also identify diagnostic inconsistencies, surface overlooked conditions and flag high-risk medication interactions that may not be apparent within fragmented data environments.
Beyond direct clinical support, AI improves operational efficiency, accelerates innovation and speeds up clinical trials by shortening patient recruitment timelines and matching eligibility criteria against unified medical and lifestyle records, thereby reducing enrollment cycles from months or years to weeks. It also lowers trial cancellation rates, supports adaptive trial design and enables continuous post-approval monitoring using real-world patient data.
The bottom line
A single, unified lifestyle record that exists alongside the clinical record enables the patient and their care team to access the same complete, clean and accurate information in terms they understand best. It offers a deeper understanding of health issues, preventative measures and available treatments.
It shifts the focus of healthcare from treatment to prevention to yield better outcomes, saving time, money, and lives.
With provider support, AI enables healthcare systems to anticipate risk, support preventative intervention and improve outcomes while simultaneously lowering costs and improving outcomes across the continuum of care.
Greg Brady is founder and CEO of Connect4Patients, a patient-centric healthcare network technology company that builds interoperable, permission-based platforms that enable patients and providers to actively participate in care and that eliminates fragmented records and siloed portals.



